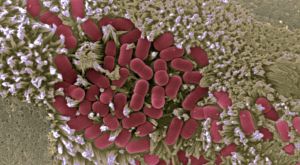
A group of researchers led by the Centro Nacional de Biotecnología of the CSIC (CNB-CSIC) has found the key to avoiding the most damaging effects of intestinal infection caused by a strain of the bacterium E. coli. The scientists observed the colonization capacity of this bacterium in the intestinal mucosa and discovered several features that could be used to develop a vaccine against this type of intestinal infection.
"The pathogenic E. coli strain we studied causes severe diarrhoea in children, with high prevalence in developing countries," says researcher Luis Ángel Fernández, from the CNB-CSIC and senior author of the paper. Fernández highlighted the importance of the discovery in this study, which has been published in the journal PLoS Pathogens. The scientists showed that for E. coli to bind to the intestinal mucosa, a group of proteins called effectors are involved in forming a lesion that destroys the intestinal microvilli, essential for nutrient absorption.
The study was carried out using enteropathogenic E. coli strains (EPEC), which are very similar to the enterohaemorrhagic E. coli strains (EHEC) that cause similar lesions and are associated with outbreaks of food poisoning in developed countries. The vaccines that could be developed might thus protect against EPEC and EHEC strains.
How do the effectors work?
The intestinal mucosa is a defensive barrier against infections. Intestinal pathogens such as E. coli have nonetheless developed specific mechanisms to bind and alter the intestinal mucosa. This generates a dysfunction in nutrient absorption and promotes the massive fluid loss that accompanies the infection. The causes of this alteration are the effectors, proteins injected by the bacterium into the human cell during infection to alter intestinal cell function.
The EPEC strains, those studied by the researchers, are a category of bacteria that mainly affects young children. This strain distinguishes itself from others by producing a lesion in the intestinal tissues called A/E (attachment and effacement), which destroys the microvilli of the intestinal mucosa.
This E. coli strain injects a large group of proteins into the intestinal cell, to manipulate cellular functions to the benefit of the infection. These proteins are the effectors. All of the EPEC bacteria have a group of effectors, responsible for the main damage to the mucosa, which are found at a point in their genome termed LEE (locus of enterocyte effacement).
There is also a larger group of effectors, scattered in different parts of the bacterium's genome, whose number varies depending on the strain. These are the non-LEE effectors. What the research team led by the CSIC found is that for the A/E lesion to be produced in the intestinal tissue, action of the non-LEE effectors is necessary.
"These results allow us to better understand the process of infection and damage to the intestinal barrier and will allow us to develop vaccines based on attenuated EPEC strains able to colonize the intestinal tissue without causing the acute symptoms of the infection," concludes Luis Ángel Fernández.
.
- Source CSIC Comunicación
- Massiel Cepeda-Molero, Cedric N. Berger, Alistair D.S. Walsham, Samuel J. Ellis, simon Wemyss-Holden, Stephanie Schüller, Gad Frankel, Luis Ángel Fernández. Attaching and effacing (A/E) lesión formation by enteropathogenic E.coli on human intestinal mucosa is dependent on non-LEE effector. PLOS Pathogens. DOI: 10.1371/journal.ppat.1006706